Cervical Health Is Preventive Health
Cervical health refers to the well-being of the lower part of the uterus — the cervix — which connects the uterus to the vagina. The cervix is routinely evaluated in clinical care to detect early changes that may lead to cancer. When cervical abnormalities are identified early through screening, treatment can be highly effective and often prevent cancer altogether.
According to the World Health Organization (WHO), cervical cancer is one of the most preventable and treatable forms of cancer when detected early and managed appropriately.
The Global Impact of Cervical Cancer
Cervical cancer continues to take lives around the world, largely due to gaps in access to preventive care:
Cervical cancer is the fourth most common cancer among women globally, with approximately 660,000 new cases and about 350,000 deaths in 2022 (WHO)
This translates to roughly one death every two minutes worldwide — over 300,000 deaths each year. (CCAE)
Nearly 90% of cervical cancer deaths occur in low- and middle-income countries, where screening and treatment services are limited. (Together for Health)
These are not just statistics. They represent mothers, daughters, sisters, and friends whose lives could often have been saved through timely screening and appropriate follow-up care.
How Cervical Screening Works
Two primary tools are used for early detection:
Pap Test (Papanicolaou Test): A clinician collects cervical cells and examines them under a microscope to identify abnormal changes (cytology).
HPV Test: Detects high-risk strains of human papillomavirus (HPV), which cause the vast majority of cervical cancers.
Both approaches are designed to identify changes before cancer develops.
Approximately 3–4% of Pap tests show abnormal cells. Most of these findings do not indicate cancer, but they do require appropriate follow-up.
It is important to note that self-collection methods are currently validated primarily for HPV testing, not for Pap cytology.
Risk Factors for Cervical Cancer
Cervical cancer does not affect all people equally. Key risk factors include:
Persistent infection with high-risk HPV strains (the primary cause of cervical cancer) (WHO)
Infrequent or inconsistent screening due to cost, access barriers, fear, or logistical challenges (Avalere Health)
Weakened immune response, including HIV infection (WHO)
Tobacco use, early sexual activity, and multiple sexual partners
Systemic barriers, such as limited healthcare access, insurance gaps, cultural stigma, and lack of trauma-informed care
These factors disproportionately affect people with fewer resources and limited access to preventive services.
Barriers That Keep People From Screening
Despite its life-saving potential, many people delay or avoid cervical screening. Common barriers include:
Pain and Discomfort
Individuals with chronic pelvic pain, anxiety, prior medical trauma, or gynecologic conditions such as endometriosis may find speculum exams painful or retraumatizing.
Logistic and Financial Burden
Screening often requires time off work, transportation, childcare, and copays. Some individuals experience repeat visits due to insufficient samples, adding further stress and expense.
Systemic Inequities
Screening rates vary widely by insurance status, geography, and socioeconomic factors. People with public insurance and those in underserved communities are screened at lower rates. (Avalere Health)
Innovation in Cervical Screening: Toward Comfort, Autonomy, and Equity
Healthcare systems must evolve to meet people where they are. Emerging approaches — including self-collected HPV testing and at-home screening options — are evidence-based tools that can expand access while respecting bodily autonomy.
Clinical studies show that self-collected HPV samples can detect high-risk HPV with accuracy comparable to clinician-collected samples. As a result, recent guidelines increasingly recognize self-collection as an option within organized screening programs.
These innovations reflect a broader scientific and clinical shift: effective cervical cancer prevention must be patient-centered, accessible, and paired with reliable laboratory analysis and clear pathways for follow-up care.
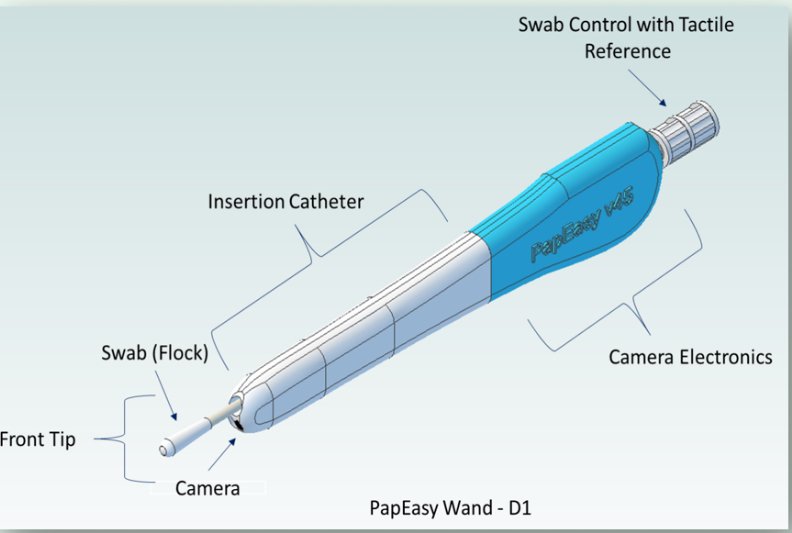
Introducing PapEasy: Screening Designed for Real Lives
PapEasy is an emerging cervical screening solution currently in development. It is designed to support HPV-based self-collection paired with laboratory testing and clinical follow-up.
PapEasy’s design goals include:
Reducing discomfort compared to traditional in-office exams
Enabling private, self-directed sample collection
Lowering practical and financial barriers to screening
Supporting participation among people who avoid exams due to pain, trauma, or access challenges
PapEasy is not yet commercially available. It does not replace gynecologic care when in-person evaluation is medically indicated. Instead, it reflects a growing movement toward expanding safe, evidence-based screening options that work within established clinical care pathways.
When paired with confirmatory testing and appropriate medical follow-up, self-collection solutions may help reach individuals who would otherwise remain unscreened.
What Happens After Results?
Receiving abnormal screening results can be stressful, but most abnormal findings do not mean cancer.
Depending on results, follow-up may include:
Repeat HPV testing
Additional Pap testing
Colposcopy (a closer examination of the cervix)
Biopsy if needed
These steps allow clinicians to monitor changes and intervene early when necessary. Timely follow-up is a critical part of cancer prevention.
The Role of HPV Vaccination
HPV vaccination is a powerful tool for preventing cervical cancer and other HPV-related diseases. Vaccination significantly reduces cancer risk, but it does not eliminate the need for screening. Regular cervical screening remains essential even for vaccinated individuals.
Taking Control of Your Cervical Health
Everyone deserves preventive care that is comfortable, affordable, and respectful.
Innovations in cervical screening — including self-collection and home-based options — are helping reduce barriers and bring care to people rather than forcing people into systems that may not meet their needs.
Whether screening occurs through a healthcare provider or through emerging patient-led tools like PapEasy, the most important factors are:
Regular participation
Evidence-based testing
Reliable follow-up care
Access to appropriate treatment when needed
Cervical cancer is largely preventable. Expanding access to high-quality screening and follow-up is one of the most effective ways to protect lives.